The Big Question… Can Kidney Disease Be Reversed?

Kidney disease can range from mild to severe, so the potential for reversal will depend on the specific cause and stage of the disease. Kidney disease is a major worldwide public health concern, affecting more than one in ten. If the kidneys become severely damaged and cannot perform their duties, advanced treatments such as dialysis or kidney transplantation may need to occur.
The question remains…can kidney disease be reversed?
This is a very contentious topic.
I will delve deeper into this question and provide research-based information to debunk the myth that kidney disease cannot be reversed.
Factors to consider
Kidney disease can be managed, and its progression can be slowed. However, whether KD can be reversed depends on many factors, including the underlying cause and the stage of the disease.
The following are some factors to consider:
- Early Stages – Within the early stages of KD, especially when the damage is due to high blood pressure or diabetes, it is possible to slow or halt the process of disease progression. Lifestyle changes, management with appropriate medication and treating the underlying condition will go a long way in supporting kidney function. If the underlying condition is addressed and managed it is possible to see improvement in kidney function.
- Advanced Stages – It is believed in the advanced stages, such as chronic kidney disease (CKD) stage 4 or 5, where kidney function is at a significant loss, complete reversal is less likely. We know that proper management, including dialysis or kidney transplantation, helps maintain a patient’s health quality.
- Acute kidney injury (AKI) – AKI is the sudden loss of kidney function. It can sometimes be reversible if the underlying cause is identified and treated quickly and appropriately. AKI can happen due to factors such as dehydration, infections, medication or kidney damage due to surgery.
- Dialysis and transplantation – It will sometimes be necessary for patients with advanced kidney disease to end up having dialysis or kidney transplantation. Dialysis helps filter waste and excess fluid from the blood when the kidneys cannot. Kidney transplantation is considered to be the most effective treatment for end-stage kidney disease.
- Lifestyle changes – It does not matter which stage of kidney disease you are at; lifestyle changes will always be of benefit. These changes may include managing blood pressure, controlling blood sugar levels, maintaining a healthy, balanced diet, staying hydrated, and avoiding harmful substances such as alcohol.
Can The Kidneys Regenerate?
Researchers at the Stanford Institute for Stem Cell Biology and Regenerative Medicine and the Sackler School of Medicine in Israel have shown that kidneys constantly grow and can regenerate themselves. This challenges decades of accepted knowledge, where it is believed that kidneys did not regenerate. It has been long thought that kidney cells did not reproduce much once they were fully formed, now, research shows that kidneys will restore and repair themselves throughout life. Findings published online on May 15 in Cell Reports indicated that the kidney is not a static organ, and it has the ability to rejuvenate itself and generate specialised kidney cells all the time.
The research, which was performed on mice, also showed how the kidney could regenerate itself. It was shown instead of one type of kidney stem cell that can replace damaged or lost kidney tissue, and there are more specialised stem cells that reside in different segments of the kidney, which will give rise to new cells within each type of kidney tissue. This research also showed that the decision these cells make to grow is made via activating a cellular pathway that involves the protein Wnt. Authors found Wnt signalling is responsible for the growth of new kidney tissue, offering a therapeutic target to promote or restore the regenerative capacity of the kidneys. Due to these findings, the authors stated, they may be able to turn on the Wnt pathway to generate new kidney-forming cells.
Adult kidneys constantly grow, remodel themselves, study finds | News Center | Stanford Medicine
Renal cell regeneration
The specialised cells within the kidneys are called nephrons. Nephrons are responsible for filtering waste and other substances from the blood. This will occur roughly every 1-2 hours. Nephrons will regenerate to a certain extent; however, their regeneration is relatively slow. Renal failure is due to the loss of structure and function of these nephrons. In humans, new nephrons (nephrogenesis) are generated until the 36th week of gestation, and no new nephrons will develop after birth. A 2020 study found in rodents, nephrogenesis occurs until the post-natal period, meaning the post-natal mammalian kidney can partly repair its nephrons.
The kidney uses intrarenal and extra renal cell sources for the maintenance repair. The authors stated that it is believed that the dedifferentiation of surviving tubular epithelial cells and the presence of resident stem cells all have an essential role to play in kidney repair. They concluded many studies have shown that stem cells from other sites, such as bone marrow, adipose and skeletal muscle tissue, umbilical cord and amniotic fluid, have potential therapeutic properties.
The repair process can be initiated in response to kidney injury or damage. Repair involves the proliferation of specific cells to replace the damaged tissue. Research also suggests there may be renal stem cells or progenitor cells in the kidneys that have the potential to differentiate into various types of kidney cells, which will contribute to the process of regeneration.
Repair and regeneration of the nephron – CIRM (ca.gov)
Kidney Regeneration: Stem Cells as a New Trend – PubMed (nih.g.ov)

Let’s look at some more studies!
A recent article published in the Science Translational Medicine has researched senescent cells and their role in renal regeneration. Senescent cells are cells that have entered a state of senescence. This is a state of irreversible growth arrest and cellular aging. In the kidneys, the accumulation of senescent cells is associated with age-related disease and aging. These cells also cause kidney scarring and impact how well the kidney can repair after injury. Senescent cells can contribute to the development and progression of kidney damage and dysfunction via the following mechanisms;
- Inflammation– Senescent cells can secrete pro-inflammatory molecules. This chronic inflammation can promote tissue damage and fibrosis in the kidneys.
- Fibrosis– Senescent cells may promote the disposition of extracellular matrix proteins, which contribute to kidney fibrosis, impairing kidney function.
- Cellular Senescence in Disease– Senescent cells have been implicated in various kidney diseases, including CKD, diabetic nephropathy and acute kidney injury.
Senescent Cells Affect Kidney Health
Mylonas et al. found more senescent cells in the kidneys of older and injured mice, also reflecting that the elderly and those with wounded kidneys have more senescent cells. Mylonas et al. studied whether these secernent cells contributed to the reduced regeneration seen in aged and injured kidneys. If the depletion of these cells using the drug, ABT-263 improved kidney function and repair after injury. They found that ABT-263 targeted senescent proximal tubule cells. This was shown in aged mouse models of acute kidney injury. Treatment resulted in improved functional recovery and reduced fibrosis. They concluded senescent cells represent a potential target to protect the kidneys.
Next, the team will study ABT-263 in human kidneys that are too damaged to use in transplant operations. They stated that if that works, the drug could be used to protect transplant recipients and patients with CKD who need operations carrying the risk of acute kidney injury.
You can read more about senescent cells in a previous article here.
Stem Cells
Stem cells also hold promise for kidney regeneration and repair. Research in this area is ongoing.
What are stem cells?
Stem cells are undifferentiated cells that have the potential to develop into various cell types within the body; this includes kidney cells. Several types of stem cells and approaches are being investigated for their potential role in the repair of kidneys.
Embryonic Stem Cells (ESCs)
ESCs can differentiate into any cell type in the body. Researchers have been exploring the potential use of ESCs to generate kidney cells. However, the clinical use of ESCs generated from surplus embryos has associated issues. This includes ethical and practical concerns, immunological rejection and the risk of teratoma.
Induced Pluripotent Stem Cells (iPSCs)
IPSCs are reprogrammed adult cells (usually skin or blood cells), that are induced to become pluripotent cells similar to ESCs. Pluripotent cells are a type of stem cell that can differentiate into any cell type except for extraembryonic cells. These cells can be directed to differentiate into kidney cells. They offer a potential source of cells for kidney regeneration.
Mesenchymal Stem Cells (MSCs)
MSCs are a type of adult stem cell found in various tissues such as bone marrow and adipose tissue. MSCs have been investigated for their potential to promote kidney repair through their anti-inflammatory and immunomodulatory properties.
Renal Progenitor Cells
These cells are more specialised in their action as they are already committed to becoming kidney cells. There has been some research focusing on identifying and identifying progenitor cells within the kidneys, which have the potential to regenerate damaged kidney tissue.

Image via Renal progenitors: Roles in kidney disease and regeneration – PMC (nih.gov)
Exosome Therapy
Most cells release tiny packets called extracellular vesicles, the most notable being exosomes. Exosomes are small but filled with high concentrations of potentially helpful substances such as RNA, DNA and proteins. Most cells release exosomes; however, researchers are very interested in the exosomes released by stem cells. Within these exosomes, the stem cells pass along the substances that make stem cells helpful in tissue repair and function.
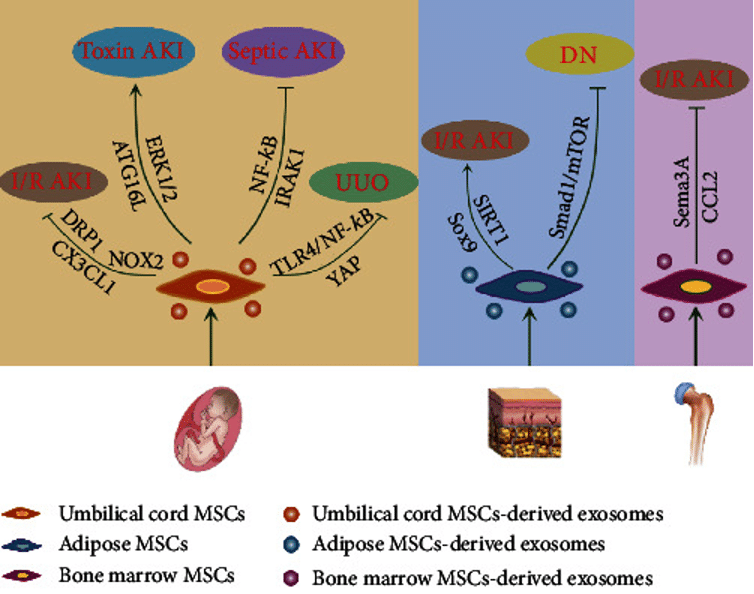
Image via Exosomes: Emerging Therapy Delivery Tools and Biomarkers for Kidney Diseases – PMC (nih.gov)
Renal Function Can Improve at Any Stage of Kidney Disease
A study published in 2013 researched this exact topic, ‘Renal Function Can Improve at Any Stage of Chronic Kidney Disease’. The study explained that even though renal function decline is considered to be relentless in CKD, improvement has been shown in those with hypertensive nephropathy. The study enrolled patients with any diagnosis of CKD stages 1 through 5.
The study found sixty-two (15.3%) patients were classified as improvers and 332 as nonimprovers. It was shown that GFR also improved in some patients with advanced CKD: 24.2% of the improvers had advanced CKD, in stage 4 or 5. Their results suggested that the ability to heal continues in advanced CKD.
The authors concluded their data showed renal function can improve over time in a significant proportion of CKD patients, even at a severe stage. Their results also suggested treating metabolic complications and 25(OH)D deficiency more effectively could promote improvement in renal function.
Renal Function Can Improve at Any Stage of Chronic Kidney Disease – PMC (nih.gov)
Lets Summaries
The narrative that kidneys cannot regenerate and that once you have CKD, there is nothing you can do about it is invalid. We have several studies showing that the cells of the kidneys can regenerate and repair themselves. From a naturopathic standpoint, if you can treat the driver of an individual’s CDK, you stop the continued damage caused to the kidneys. That is step one. Once you have that under control, you can support the healing of the kidneys by reducing inflammation and oxidative stress, reversing fibrosis, and removing senescent cells. Sometimes, a patient may need two or more of these approaches to initiate an improvement in kidney function. Our point? If you treat the person as an individual and not just a disease, it is possible to reverse and improve kidney function.
There’s a lot of information here! I hope you found it inspiring and helpful!
If you have found this helpful article, please share it with your family or friends or head to our Facebook page and leave us a comment. We would love to hear from you.
Share This Article
LIKE WHAT YOU’VE READ?
Sign up for free updates delivered to your inbox. Join our community and get tips on health, wellness, nutrition, and more.
More From Our Blog

The Oral Microbiome & Chronic Kidney Disease
The oral microbiome plays an essential role in the incidence and development of

Natural Therapies In The Treatment of Polycystic Kidney Disease
Regarding dietary interventions in treating and managing PKD, the science is solid. The
What Causes Cyst Formation In Polycystic Kidney Disease?
What is polycystic kidney disease? Polycystic kidney disease (PKD) is a prevalent genetic
Bicarbonate Supplements? Is It The Best Way To Alkalize in Kidney Disease?
Throughout the ages, human diets have undergone a significant transformation, shifting from an
SS-31 Peptide and Kidney Disease
Kidney disease is a global health concern. The kidneys, especially the proximal tubules,

The Role of Calcium in Kidney Disease
Calcium is the most abundant mineral in our body; ninety-nine per cent of




